Difference Between Extrinsic And Intrinsic Blood Clotting Pathways
 David Perry
David Perry 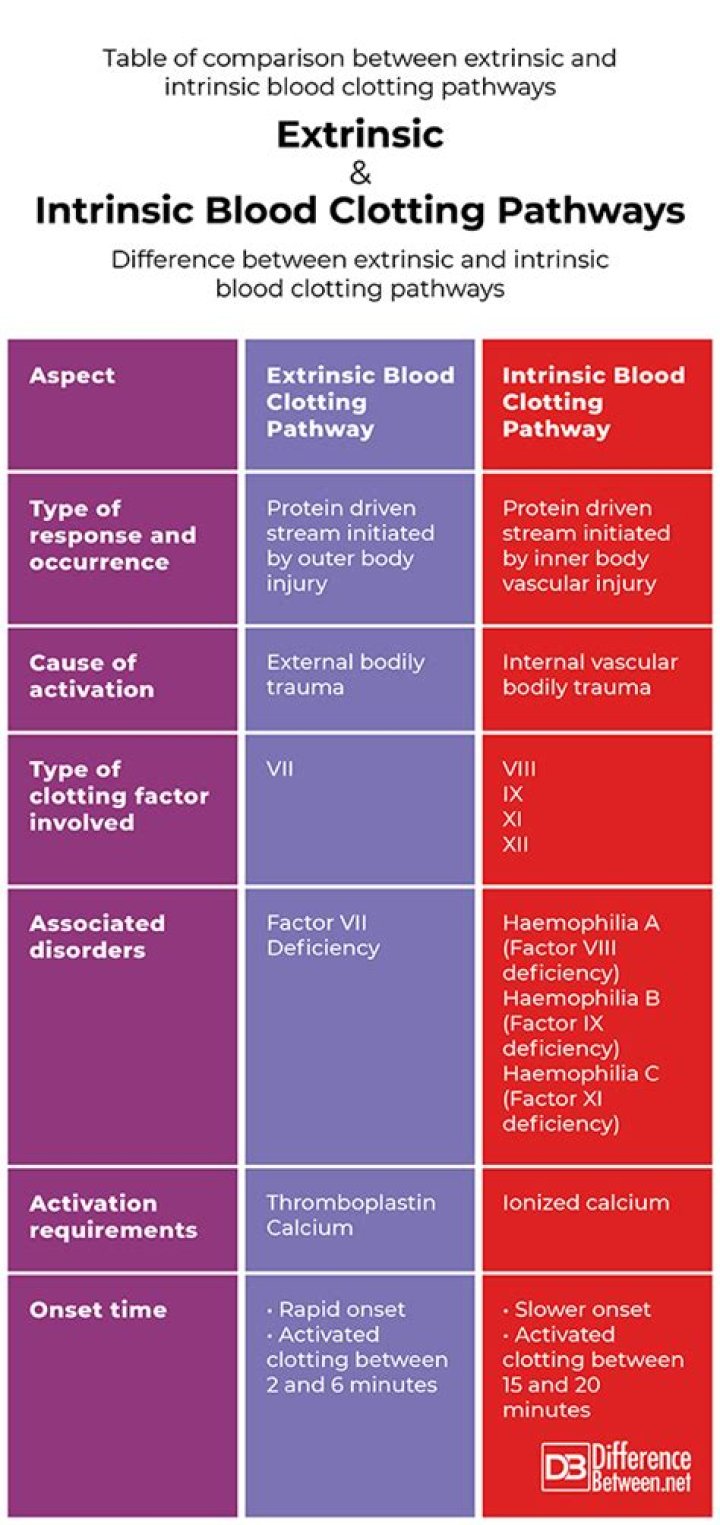
Blood clotting is a complex process essential to our body’s ability to stop bleeding. There are two pathways by which blood can be clotted: the extrinsic pathway and the intrinsic pathway. These two pathways work together to form a fibrin clot, which is the final product of blood clotting. In this article, we will discuss the differences between the two pathways and how they interact to form a fibrin clot.
What is the Extrinsic Pathway?
The extrinsic pathway, also known as the tissue factor pathway, is the faster of the two pathways and is triggered by outside factors such as tissue damage. This pathway is triggered by the release of the enzyme tissue factor from damaged cells. This enzyme binds to Factor VII and activates a cascade of reactions that ultimately lead to the formation of a fibrin clot.
What is the Intrinsic Pathway?
The intrinsic pathway, also known as the contact activation pathway, is slower than the extrinsic pathway and is triggered by contact with a foreign surface. This pathway is triggered when Factor XII comes into contact with a foreign surface and activates a cascade of reactions that ultimately lead to the formation of a fibrin clot.
Difference between Extrinsic and Intrinsic Pathways
The main difference between the extrinsic and intrinsic pathways is the way they are triggered. The extrinsic pathway is triggered by tissue damage while the intrinsic pathway is triggered by contact with a foreign surface. Additionally, the extrinsic pathway is much faster than the intrinsic pathway. The extrinsic pathway is initiated within seconds while the intrinsic pathway can take up to several minutes.
Interaction between Extrinsic and Intrinsic Pathways
The extrinsic and intrinsic pathways work together to form a fibrin clot. The extrinsic pathway is activated first, triggering the release of Factor VII and the subsequent cascade of reactions. The intrinsic pathway is then activated by contact with a foreign surface and triggers the release of Factor XII, which activates a cascade of reactions that lead to the formation of a fibrin clot.
Factors that Affect Blood Clotting
There are a number of factors that can affect the rate and quality of blood clotting. These include the amount of tissue damage, the presence of anticoagulants in the blood, the presence of platelets, the temperature, and the pH of the environment. Additionally, genetic factors can also influence the rate and quality of blood clotting.
Role of Platelets in Blood Clotting
Platelets are essential for the formation of a fibrin clot. Platelets are activated by the extrinsic and intrinsic pathways and then bind to the exposed collagen on the damaged tissue. This helps to form a platelet plug, which stops the bleeding. The platelet plug is then strengthened by the formation of a fibrin clot.
Role of Calcium in Blood Clotting
Calcium is essential for the formation of a fibrin clot. Calcium ions are required for the activation of the extrinsic and intrinsic pathways and are also necessary for the activation of the enzyme thrombin. Thrombin then converts the soluble fibrinogen into insoluble fibrin, which is the main component of a fibrin clot.
Role of Vitamin K in Blood Clotting
Vitamin K is essential for the formation of a fibrin clot. Vitamin K is required for the activation of several clotting factors, including Factors II, VII, IX, and X. These factors are essential for the formation of a fibrin clot.
Role of Anticoagulants in Blood Clotting
Anticoagulants are substances that inhibit the formation of a fibrin clot. These substances bind to clotting factors and prevent them from activating the extrinsic and intrinsic pathways. Examples of anticoagulants include heparin, warfarin, and aspirin.
Role of Fibrinolytic Enzymes in Blood Clotting
Fibrinolytic enzymes are substances that break down existing fibrin clots. These enzymes break down the fibrin strands, which allows the blood to flow freely. Examples of fibrinolytic enzymes include plasmin and streptokinase.
Role of Endothelial Cells in Blood Clotting
Endothelial cells are cells that line the inner walls of blood vessels. Endothelial cells produce a variety of substances that regulate the formation of a fibrin clot. These substances can stimulate or inhibit the extrinsic and intrinsic pathways and can also affect the activity of platelets and clotting factors.
Role of Thrombin in Blood Clotting
Thrombin is an enzyme that plays a key role in the formation of a fibrin clot. Thrombin is activated by the extrinsic and intrinsic pathways and is responsible for converting soluble fibrinogen into insoluble fibrin. Fibrin is the main component of a fibrin clot.
Role of Blood Plasma in Blood Clotting
Blood plasma is the liquid component of the blood and is essential for the formation of a fibrin clot. Blood plasma contains the clotting factors, platelets, and other substances that are essential for the formation of a fibrin clot.
Role of Blood Cells in Blood Clotting
Blood cells, including red blood cells and white blood cells, are essential for the formation of a fibrin clot. Blood cells help to transport the clotting factors and platelets to the site of injury and can also help to activate the extrinsic and intrinsic pathways.
Conclusion
In conclusion, the extrinsic and intrinsic pathways are two distinct pathways that work together to form a fibrin clot. The extrinsic pathway is triggered by tissue damage while the intrinsic pathway is triggered by contact with a foreign surface. The extrinsic pathway is faster than the intrinsic pathway and is activated within seconds. Additionally, platelets, calcium, vitamin K, anticoagulants, fibrinolytic enzymes, endothelial cells, thrombin, blood plasma, and blood cells all play a vital role in the formation of a fibrin clot.



